GYNAECOLOGICAL CONDITIONS
I can help women with all aspects of gynaecological problems. My areas of expertise include management of fibroids, endometriosis, ovarian cysts, polyps and abnormal uterine bleeding.
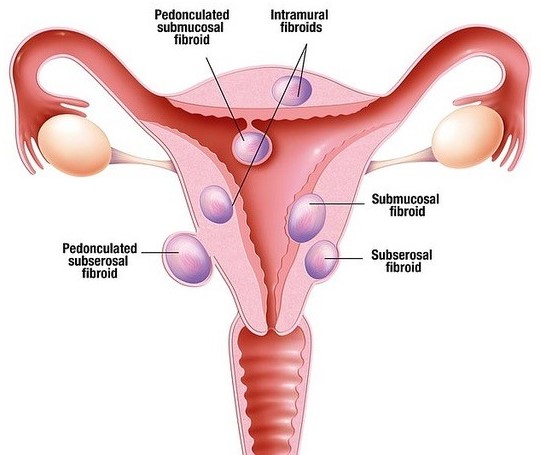 |
FIBROIDS Fibroids, also known as leiomyomas, are benign tumours made up of smooth muscle cells. They usually arise in the uterus but rarely can occur elsewhere in the pelvis. Women with fibroids may experience symptoms such as: • Heavy or prolonged menstrual bleeding • Infertility • Miscarriages • Pressure effect on nearby organs, such as the bladder (causing frequent urination) and bowel (causing constipation) • Pelvic pain • Being able to see and feel a firm abdominal mass Treatment of fibroids may include medical therapy, interventional radiological procedures, or surgery. The size, number and location of the fibroid(s) as well as the woman’s desire for fertility or uterine conservation also have an impact on management. |
 |
ENDOMETRIOSIS Endometriosis is a condition whereby the tissue which normally lines the uterine cavity (called the endometrium) grows in locations outside of the uterus. These “endometrial deposits” respond to stimulation by our natural hormones to grow and shed (bleed) during the menstrual cycle the same way that the normal endometrium grows and sheds within the uterine cavity. Bleeding which occurs outside of the uterus (and within the abdominal cavity) leads to inflammation, pain, and formation of scar tissue. Women with endometriosis usually present with three main problems: 1) Period abnormalities Endometriosis is very common and affects around 1 in 10 women in the reproductive age range. It can cause severe symptoms leading to iron deficiency anaemia, missing school or work due to pain, relationship problems, depression and reliance on painkillers. The diagnosis of this condition may require specialised ultrasound scans, MRI scans and laparoscopic (keyhole) surgery. Treatment of endometriosis can be complex and depends on the presenting symptoms and whether fertility is a main concern. Often medical (hormonal) therapy is used in conjunction with surgery. Some women with longstanding endometriosis may require other treatment such as pelvic floor physiotherapy, clinical psychology, fertility treatment and assessment by a pain specialist. |
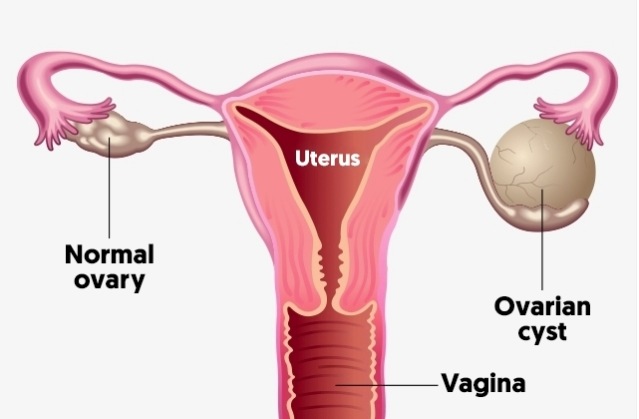 |
OVARIAN CYSTS Cysts are fluid-filled growths that affect the ovary, but sometimes also occur in and around the fallopian tube. Ovarian cysts can be benign or malignant (cancerous), therefore specialised scans such as pelvic ultrasound, CT or MRI scans, and blood tests may be required prior to surgery. Most cysts are benign, come and go with the menstrual cycle, and do not cause any symptoms. However, ovarian cysts that are large (5cm or greater) can become complicated by haemorrhage, rupturing or twisting, necessitating emergency surgery. Large ovarian cysts can be removed electively via laparoscopic surgery to prevent such complications. There are some specific cysts such as endometriomas (chocolate cysts) and dermoid cysts (which can contain various tissue types including fat, skin, hair, teeth and bone) which do not go away on their own. Such cysts are also able to be removed via laparoscopic surgery. |
 |
ABNORMAL UTERINE BLEEDING Abnormal uterine bleeding includes heavy periods (menorrhagia), bleeding in between periods and post-menopausal bleeding.Menorrhagia and inter-menstrual bleeding can be secondary to many different causes such as: • Fibroids • Adenomyosis • Polyps • Endometrial hyperplasia (thickening of the uterine lining with abnormal precancerous cells) • Hormonal imbalance • Cancer All cases of post-menopausal bleeding should be investigated to rule out cancer, but many cases may be due to post-menopausal changes or polyps. A proper diagnosis is required before treatment can be considered. Diagnosis will usually require blood tests, pelvic ultrasound scans or other specialised scans such as CT or MRI. In some cases, a minor surgical procedure called hysteroscopy may be required to diagnose and treat the cause. Hysteroscopy is a minimally-invasive procedure where a camera is inserted vaginally, passed through the cervix and into the uterine cavity to allow direct visualisation of the cavity. Treatment is directed at the underlying cause of the abnormal bleeding and may involve medication, interventional radiology and further surgery. |
 |
ABNORMAL CERVICAL SMEARS
The Cervical Screening Test (CST) replaced the Pap smear test in Australia in December 2017. Having routine cervical screening is the best protection against cervical cancer, one of the most preventable cancers in women. The CST is more effective at preventing cervical cancer than the previous Pap smears as CSTs not only look for abnormal cells but they also detect the human papillomavirus (HPV) which can cause cell changes that may progress to cervical cancer. If you are aged 25 to 74, your first CST is due two years after your last Pap smear. If your CST is normal, you will only need to have the test every five years from then on. Some abnormal CST results are recommended to be further assessed with a procedure called colposcopy. |
 |
PELVIC ORGAN PROLAPSE
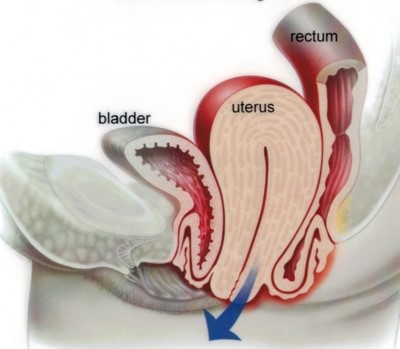
Weakness of the pelvic floor muscles and ligaments can lead to dropping down of the pelvic organs towards the vaginal opening. The structures involved may include the uterus, vagina, bladder and rectum. In some cases the pelvic floor organs may protrude outside of the vagina. Many women with prolapse do not have symptoms and may not require treatment. Those who do experience symptoms may present with: Treatment may involve weight loss measures, pelvic floor physiotherapy, vaginal support pessaries, and surgery. |

